Life Under the Microscope
The monitoring, testing, and medical rituals that quietly shape your life.
If you’re just joining the ride, I recommend starting from the beginning. Each post builds the trail that led me here.
A quick note before you dive in: This post contains medical details and personal procedures related to UC. It’s not graphic, but it’s honest — because this too is part of the story.
By now, you’re probably imagining UC through its symptoms — the bathroom trips, the cramps, the exhaustion, the unpredictability. But there’s another part of the disease that runs quietly in the background, shaping everything you do: monitoring. Testing. Scanning. Measuring. Watching.
A constant loop of medical checkpoints designed to track inflammation, prevent complications, and determine whether the drugs meant to help are actually working.
That part of the story develops its own rhythm: appointments, lab slips, prep days, follow-ups, more appointments. For more than two decades, this was as much a part of my life as cycling.
Back when I was first diagnosed, none of that was really on my mind. I took it in stride, moved on, and assumed I’d just cope. And for a while, I did.
Then the tests started stacking up.
I had my first colonoscopy at 37. After that, they became routine — every one to three years, depending on how I was doing. I’ve honestly lost count of how many I’ve had. I used to joke with the nursing staff and my doctors that I deserved a “frequent buyer card” so that every tenth one would be free.
No matter how many you’ve had, they’re never fun. You learn to adapt to the prep, the waiting, and the procedure because there isn’t another choice.
Bloodwork followed the same path. At first it felt occasional. Then it became expected. Every flare meant more vials. Every medication change meant baseline labs followed by more labs. Over time, blood tests became like weather reports — they didn’t tell you exactly what would happen, but they gave you a sense of what kind of day, or month, you might be heading into.
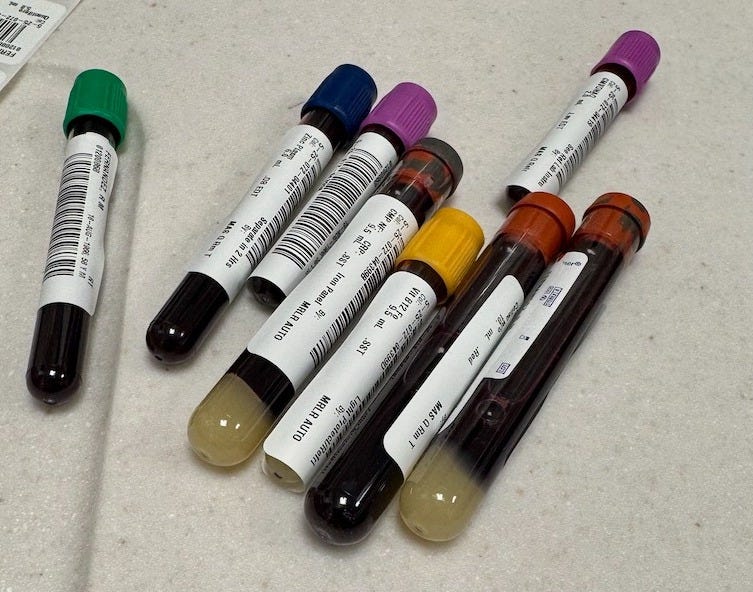
They measured everything: inflammation markers, blood counts, anemia indicators, liver and kidney function, drug levels, infection markers, nutritional deficiencies. I lost track of how many vials I’ve given over the years.
Eventually, bloodwork became a language — one you learn to read almost as well as your doctor. Sometimes the numbers told me things I didn’t want to hear. After nearly five years on Infliximab, labs showed rising inflammation markers even though I had been in remission. Quietly, steadily, the data made it clear my body had begun to lose its response to the medication. The drug wasn’t working anymore, and a flare was brewing.
Because of long-term medication and chronic inflammation, the testing didn’t stop at blood draws. Bone density scans. Liver and kidney screenings. Eye exams. Dermatology checks. Cancer surveillance. Tests most people my age wouldn’t even consider until much later in life.
I remember being 45 and getting a bone density scan typically reserved for people in their 60s or 70s. It was humbling — and unsettling. Knowing I may have been more susceptible to fractures changed how I rode. I thought twice before tackling descents and obstacles that once felt effortless. Not fear exactly — just another quiet calculation layered onto everything else.
The medications themselves also changed how I moved through the world. Infliximab suppressed my immune system. While it reduced inflammation, it made infections more dangerous and recovery less predictable. Long before COVID, I was already masking. During a work trip to Japan in 2018, I bought a reusable mask simply because I was tired of the generic surgical ones I’d already been wearing. When COVID hit, I already had N95s in my dresser drawer — and ended up sharing them with friends when supplies ran short.

Bloodwork also explained symptoms I never would have connected on my own. Fatigue I had blamed on flares or poor sleep turned out to be anemia from chronic blood loss. I’ve had mild tinnitus for years, something I always attributed to my time in the Army or long days mowing polo fields in Dickerson, Maryland with Led Zeppelin blasting at full volume. But during severe flares, it changed. The sound became rhythmic, pulsing, intrusive. Pulsatile tinnitus, it turns out, can be linked to anemia. Another reminder that UC doesn’t stay politely confined to the colon.
Then there were the painful red bumps that appeared on my legs — erythema nodosum, an extraintestinal complication of UC. They first showed up during a summer trip to Peru, when wearing long pants in the heat was ridiculous, but so was letting people see what my legs looked like. The embarrassment was immediate. What’s wrong with your legs? Have you tried moisturizer? One friend even joked, “Looks like AIDS…” Not funny. Just one more thing to manage, explain, and quietly carry.
Over time, I learned how to read my results. Not in a way that gave me control — nothing ever did — but in a way that gave me context. I could tell where I was in a flare, whether relief was likely, or whether I was just buying time. The numbers didn’t make things easier. They just made it harder to lie to myself.
Bloodwork doesn’t offer comfort. It offers confirmation.
It confirms that what you’re feeling is real. That the exhaustion isn’t imagined. That the pain has a source. And eventually, it confirms when doing everything you’re supposed to do still isn’t enough.
That realization didn’t arrive all at once. It came vial by vial, scan by scan, result by result — until pretending I could outthink or out-manage this disease became harder than accepting what the data had already made clear.
This post reflects personal experience. A medical disclaimer is available on the About page.